Last Updated on by SiteControl
Do you need help choosing the best Indiana health insurance coverage for yourself and your family? We realize that reviewing dozens of different 2025/2026 Marketplace medical plans from the major companies is not easy. For that reason, we utilize the nation’s top quote engine, so that researching price and coverage becomes a simple process. And we highly recommend that you ask our advice when comparing your options. Anthem Blue Cross, Ambetter, Aetna, CareSource, Cigna, and UnitedHealthcare offer Obamacare plans. Many additional carriers provide Senior Medicare coverage.
With our four decades of experience and non-biased opinions, you maximize your savings. We carefully compare each option that is available, and base our ratings solely on rates, benefits, customer feedback (like yours!), and other industry insider opinions and comments that pertain to these policies. Single and family plans (Metal) consist of four choices and a “catastrophic” option for younger applicants, or others with specific financial concerns. Both Affordable Care Act and non-Obamacare policies are offered. Short-term plans do not contain all mandated essential health benefits, but provide a flexible low-cost alternative that is appropriate in several situations.
Senior healthcare coverage is provided by original Medicare, so Marketplace rules and regulations are mostly not applicable. Although Medigap supplement, Advantage, and Part D prescription drug plans help reduce out-of-pocket expenses, unless you have reached age 65 and are Medicare-eligible, Exchange contracts are not applicable. All Supplement plans offered by carriers are standardized, and are offered in Letters A-N. There are no new policy options for E, H, or I. A high deductible (HD) option is offered for Plan F (current plan owners) and Plan G. Rates for HD plans are typically substantially less than most other plans.
Many households will have one spouse that is Medicare-eligible, while the other spouse has not reached age 65. The federal subsidy is based on the total household income, so the older spouse’s income (including pension or retirement) must be considered. Once both spouses have reached age 65, any Medigap plans that are issued will be approved separately, since Senior policies are always single plans. It is also possible for each spouse to be covered by a different carrier and plan, and with different levels of benefits. For example, one spouse may enroll in a Supplement plan, while his/her spouse enrolls in an Advantage plan. Part D prescription drug plans are often not needed when enrolled in an Advantage plan.
Plan Differences (Under Age 65)
With more than 40 years of helping customers and investigating carriers, we’re here to guide you through the process of researching, finding, applying, and enrolling for a policy. We teach you the difference between an HMO, EPO, PPO, POS, and an HSA, and show you rates from all of the top-rated companies. US Health And Life, Medical Mutual, and PHP no longer offer personal Marketplace (On-Exchange) plans in the state, so we have deleted them from our under age-65 database. UnitedHealthcare has returned to the Hoosier State as they since they rejoined several other states within the last few years. IU Health Plans offers Senior Medicare products, but not ACA options.
We have also removed plans that are not considered “real coverage,” including the cheap discount and limited-benefit contracts. These types of plans often have vague coverage descriptions, many exclusions, and non-refundable application/enrollment fees. High-pressure sales techniques are typically used when these plans are marketed and sold. Often, boiler room operations market “limited benefit” policies, and the retention rate is extremely low. It is generally not possible to meet (in person) the representatives that market these contracts. Refunds of coverage are typically very difficult to obtain in a timely manner.
The Marketplace (it began 11 years ago) has fewer options available than in previous years, but also includes a federal tax subsidy credit. Qualification is based on household income (Federal Poverty Level) instead of the medications you take or what conditions you currently have. Your “Modified Adjusted Gross Income” (MAGI) determines the exact amount you receive, which is instantly deducted from the premium. This “credit” is not taxable, although you are required to estimate your new projected income each year. Changes in your employment/income and family makeup can impact the level of your subsidy.
By 2027, additional low-cost customized options may become available, depending on the passing of specific legislation. Designed for healthy applicants age 50 and older, prices would be more affordable than current plans. Non-compliant options will continue to be offered to all applicants under age 65. Stand-alone dental and vision coverage and other ancillary policies can also be easily purchased. Short-term plans can also be customized to add extra benefits, although many exclusions and limitations are included. Note: Federal subsidies have substantially increased since 2023, so many middle-income and high-income households are receiving financial assistance.
Smoking Counts But Your Weight Doesn’t
Smoking (nicotine usage) continues to impact the price you pay, although your BMI (height and weight) is no longer relevant. Whether you weigh 140 or 640, your premium is not impacted. Many “temporary” policy applications also do not ask you to disclose your height and weight. However, any associated medical conditions that involve continuous treatment, may require you to select a more expensive plan (Silver tier instead of Bronze tier) to avoid high out-of-pocket expenses. Reviewing the retail cost of your medications is also highly recommended.
Although any side-by-side analysis of medical plans must include the cost, we feel it is equally important to ensure you understand how benefits and exclusions differ from one plan to another. Each policy is different, and while it is very difficult to review every page of the contract, we take the time to point out the coverage, benefits and exclusions that are likely to affect you the most. Many carriers do not offer plans in all counties, and their provider network may not be countrywide.
The best policy for someone else may not be the best policy for you. Households may also split plans to better accommodate specific health conditions or provider needs. Dependents who reach age 26 are generally required to apply for an individual plan. An SEP allows them to qualify for guaranteed coverage regardless of health conditions.
NOTE: Generally, exclusions are similar on most Marketplace plans. Non-approved experimental surgery and treatment that is not medically necessary are not covered. Services completed by out-of-network providers may also result in large out-of-pocket expenses, subject to the policy limits. Major medical benefits are covered, but often subject to a deductible and coinsurance. Many PPO options are offered, but HMO plans are more restrictive when seeking treatment outside of the network. EPO plans have become more popular in recent years.
How We Provide Prices

Our quote engine provides cost and coverage information that is updated daily and allows Indiana consumers to create multiple scenarios in seconds. We realize that many applicants will prefer a high-deductible catastrophic plan, while others may prefer a traditional comprehensive plan with low copays. And if you need to schedule a surgery and pay the lowest possible out-of-pocket expenses, there are specific policies that will help you, especially during Open Enrollment. Currently, $9,200 is the maximum out-of-pocket expenses (per person) on Marketplace plans.
Maximum out-of-pocket expenses can be lowered if a Silver or Gold-tier plan is selected. Platinum plans are the most expensive options, but may not be cost-effective unless you are being treated for chronic conditions. Generally, the insurer pays 90% of expenses while the policyholder pays about 10%. Shares of expenses are paid earlier than all other tiers. HSAs (see below) should be considered for individuals or families that typically have few medical expenses. Note: Platinum-tier contracts are not offered by most carriers.
Indiana Health Savings Accounts
Health Savings Accounts have become increasingly popular and are one of the most widely-viewed plans from customers. Since so many benefits are now mandated (legally required), many individuals and families are choosing options that maintain lower premiums, but also place deductibles and higher out-of-pocket expenses on coverage you may not need (maternity, for example). When eligible for Medicare, HSA accumulations can be utilized for specific expenses.
HSAs also allow policyholders to pay for medical, vision, and dental expenses with pre-tax dollars. This includes in-network and out-of-network expenses. Currently, the maximum allowed 2025 contribution is $4,300 for an individual and $8,550 for a family. The minimum allowed deductibles for the required accompanying HDHP plans are $1,650 for an individual and $3,300 for a family. Note: for 2026, HSA contribution limits are $4,400 for individuals and $8,750 for family coverage. Minimum allowed deductibles increase to $1,700 (single) and $3,400 (family). Maximum out-of-pocket expenses are $8,500 per person and $17,000 per family.
As you consider these different options, we are always available, via phone or email to offer our expert advice, and make sure the policy you select is going to meet your needs at a cost that won’t send you into sticker shock! If your income has reduced this year, you’ll be entitled to receive a bigger subsidy. However, a significant increase in household income may require you to change plans to maintain similar benefits and out-of-pocket expenses. The income of a Medicare-eligible spouse must also be included in the subsidy calculation.
Underwriting Factors Impact Cost Of Plans
Any Indiana health insurance comparison must take into account the underwriting guidelines of each company. For example, taking high blood pressure medication (or any drug) will not impact the rate. However, specific carriers may charge differently for nicotine use, since it is the only underwriting factor. In recent years, the surcharge for smoking has dramatically increased. Serious medical conditions such as heart disease and cancer once required a “guarantee issue” (GI) policy. This is not needed any longer with the passage of “The Affordable Care Act.”
Despite not being a medical-related factor, the county of residence will influence the cost of coverage. Also, there can often be a large difference in the number of companies that offer Marketplace plans. With UnitedHealthcare, Anthem Blue Cross And Blue Shield, Cigna, Humana and Aetna exiting the private healthcare market in the state, fewer policy choices are now available. Although Anthem and other carriers continue to offer Group and Senior coverage, prices will continue to increase for persons under age 65 if other companies continue to exit the market.
With only six carriers (Anthem, Aetna, US Health And Life, Ambetter and CareSource) remaining, more companies will hopefully offer Exchange plans in the future. UnitedHealthcare offers popular short-term plans (through Golden Rule) and may re-enter the Marketplace in the future with market Exchange options. Many Hoosier residents would also like to see Aetna to start offering plans again.
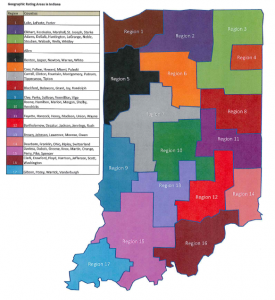
Geographic Rating Areas
There are 17 different rating areas in the state. Each region consists of at least three counties with the exception of Region 4, which contains only Allen County. Region 15 is one of the biggest zones (located in Southwestern Indiana), including nine different counties.
Previously, 2-4 companies offered 20 plan choices (or more) in each Region. Rating area 14, however, only offered one choice (Anthem BCBS). The counties in this area are Dearborn, Franklin, Ohio, Ripley and Switzerland. Six other areas offered only two carriers while three areas (2,3 and 4) offered four different companies and more than 60 different policy choices. The State Department Of Insurance provides a graphic (see below).
Indiana’s Exchange Enrollment History
In the second year of the Exchange, enrollment peaked, However, since 2014, the number of enrollees has steadily declined. Medicaid expansion six years ago was a factor, since it allowed many lower-income households to apply for government assistance instead of purchasing a Marketplace plan. Other factors impacting declining enrollments include shorter OE period, increased popularity of temporary plans, removal of mandate penalty, and higher rates for non-subsidized plans. Yearly enrolled persons are shown below:
2014 – 132,000
2015 – 218,000
2016 – 196,000
2017 – 174,000
2018 – 166,000
2019 – 148,000
2020 – 140,000
2021 – 136,000
2022 – 156,926
2023 – 185,354
Guarantee Approval Options
Until seven years ago, A “GI” plan provided needed treatment faster than an underwritten option. Since they were often approved in two weeks or less, it was necessary to utilize them if treatment was immediately needed or there was a life-threatening situation. Now, other than temporary coverage, unless you don’t meet citizenship requirements or are eligible for Medicaid or Medicare, you should be quickly approved. A policy number and effective date should be received (in writing) to verify the policy is active. Online verification is also offered.
HIP 2.0
Many low-income earners in the state have been helped by the original HIP 2.0 plan to cover more residents that are without coverage. More than 300,000 persons became eligible for this state-sponsored plan instead of Medicaid. Taxes from the sale of cigarettes and additional hospital revenue have helped fund the project. NOTE: You must be between ages 19 and 64 to apply for benefits. You may also apply for private plans at their full retail cost.

Referred to as “HIP 2.0,” it is designed to help persons that fall within 22% and 100% of the Federal Poverty Level (FPL). Hoosiers above 100% are able to qualify for policies through the Marketplace that will provide robust benefits, including mental health, maternity and pediatric dental. However, large changes in income, or job-loss, can result in HIP 2.0 eligibility.
HIP “Basic” and a HIP “Plus” account cover everyone up to the 138% FPL level. The Plus option provides the best value and is for persons above the 100% level and they would be required to make small premium payments. A POWER account receives monthly contributions based on the household income. Typically, ER visits are the only service that requires a copay.
The Basic option does not include dental or vision benefits and requires more out-of-pocket copays. If your income is up to $16,590 ($22,371 for couples), you may qualify. If you take advantage of free preventative benefits, you may be eligible for additional compensation. POWER contributions are not made, and office visit copays are between $4 and $8. Hospital visit copays may be as high as $75, which is still lower than Marketplace contracts. The preferred drug and non-preferred drug copays are $4 and $8.
Private Vs. Group
It’s also important to understand the distinction between a private vs. group plan. Many of the mandated benefits are completely different and numerous extensions have been granted to employer-based policies. Also, not all business owners are required to offer medical benefits to their workers. The number of employees has a major impact on employer obligations. However, all HIPAA rules still apply, so your privacy is protected. Exchange contracts are all “GI.”
A major difference between a personal and work-provided policy is the process of selecting and enrolling. When your employer offers benefits, although there may be multiple choices, the total availability of plans will be much less than shopping for a policy through the Marketplace. Also, although your employer may offer to pay a portion of your premium, you are ineligible for federal subsidy compensation unless you leave the employer or no longer meet the qualifications to purchase any of their plans.
SHOP (Small Business Health Options Program) plans for small business coverage (1-50 employees) offer customizable options with flexible premiums. Dental coverage is also available. Hoosier State premiums are generally very competitive compared to other states. Indiana SHOP rates are published online. Non-profit organizations are also eligible for coverage.
A SHOP small business health care tax credit may be offered if less than 25 full-time employees earn less than an average of $50,000. Applying and enrolling is a simple process through an approved insurer or licensed broker. The credit is 50% of the cost for employee premiums and 35% if the company is classified as non-profit. The average worker salary should be approximately $50,000 or less.
However, if you lose employer-based coverage as a result of job termination, regardless of what month it occurs, you automatically qualify for a “Special Enrollment Period,” which allows you to buy guaranteed coverage with any applicable subsidy. You typically are given about two months to determine which policy to buy. Naturally, we’ll work with you to select the best offer. Your coverage continues to January 1, when you can continue the plan (unless the carrier no longer offers the policy), or apply for a different plan.
ICHIA No Longer Available
Until the “Exchange” was ready, the “ICHIA” acted as a high-risk pool, so that individuals and families had the opportunity to buy a policy despite adverse medical history. Prices were higher than a typical personal policy but were very attractive when put side by side with another state’s program. Although the application and approval process could take as long as 90 days, coverage was guaranteed, with no waiting period. The policy could be terminated by the insured at any time.
But state high-risk pools are no longer needed. Every person has an opportunity to shop, compare, and enroll in a plan that is eligible for government assistance. Throughout the year, special enrollment periods are offered in the event of divorce, loss of job, birth of a child and many other situations. Once you reach age 65, Medicare eligibility will eliminate your need to purchase Marketplace policies. All Supplement plans are standardized, which simplifies the comparison process for Indiana Medigap coverage.
We urge you to utilize our website for free Exchange quotes and comparisons. Our knowledge and experience will help you easily compare and quickly find the best solution to your needs. We have created links that offer you choices of applying for a policy directly to the carrier or with the free help of an experienced broker. There is never a cost or obligation for using our personal or website help.

